The big announcement this week from Medicare — setting forth specific targets for a historic shift away from fee-for-service reimbursement in order to reduce costs and improve quality — is less than it seems.
Medicare has been talking about value based purchasing for decades now, and thus far has taken baby steps towards implementation. Even the strides taken in recent years, and the targets laid out this week for the future, don't really leave FFS medicine in the dust. ACOs and other MSSP innovations don't entirely move away from FFS reimbursement; they just add cost and quality kickers as part of a retrospective reconciliation.
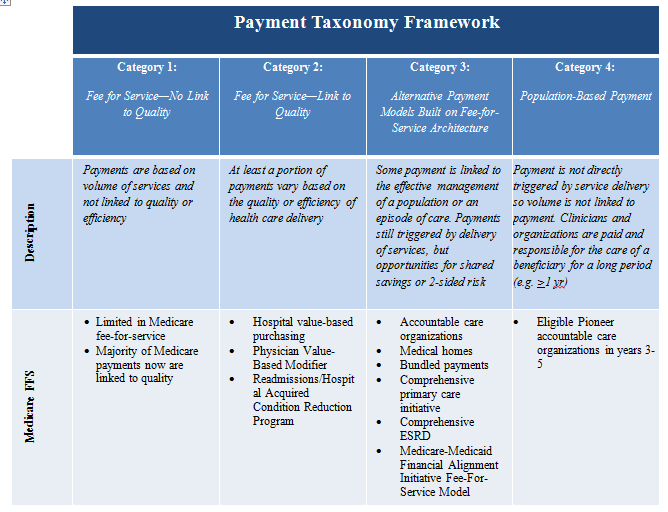
CMS identified four categories of payment and targets related to each of these categories.
- category 1—fee-for-service with no link of payment to quality
- category 2—fee-for-service with a link of payment to quality
- category 3—alternative payment models built on fee-for-service architecture
- category 4—population-based payment
These categories are explained further in the chart below:
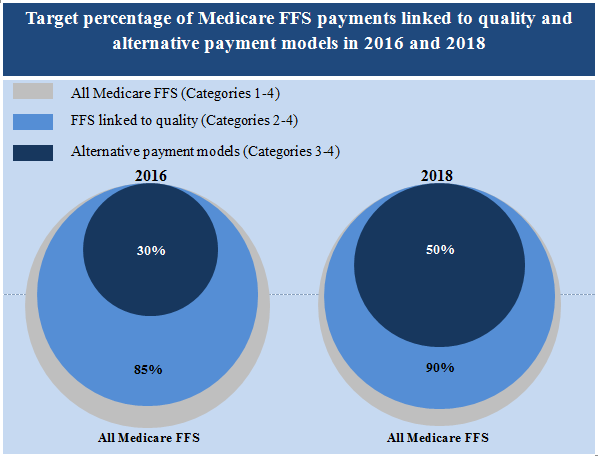
The targets over the next few years are set forth in the graphic below:
True population-based payment — just a slice of category 4 — represents only a fraction of the smallest category shown in this chart.
CMS's new spin on the Triple Aim is explained thus:
To achieve better care, smarter spending and healthier people, we are focused on three key areas: (1) improving the way providers are paid, (2) improving and innovating in care delivery, and (3) sharing information more broadly to providers, consumers, and others to support better decisions while maintaining privacy.
Again, these are laudable goals, but the announcement should have been presented as more evolutionary than revolutionary.
Not to be outdone, "[t]he Health Care Transformation Task Force, whose members include six of the nation’s top 15 health systems and four of the top 25 health insurers, challenged other providers and payers to join its commitment to put 75 percent of their business into value-based arrangements that focus on the Triple Aim of better health, better care and lower costs by 2020."
OK, so we know that this is where the ship is headed. The question for the provider community is: Now what?
Well, folks, now you need to start thinking even more seriously about how to manage population health under a global payment mindset. To get the juices flowing, take a look at a couple of HealthBlawg resources: A post entitled Health Care Innovation: Primary Care is the New Black, and a slidecast, The Camel's Nose is in the Tent: How Provider Organizations Can Succeed under Health Reform, laying out ways in which one's thinking needs to evolve in order to be ready to play in this sandbox.
There are a variety of tools for communicating about and managing care (follow link for info about one example – a client) as well as measuring outcomes, and strategies to build on the data collected and managed using these tools, that provider organizations, big and small, can use in order to prepare for and participate in this slow-motion transformation of the American health care system.
What are YOU going to do?
You know where to find me …
David Harlow
The Harlow Group LLC
Health Care Law and Consulting